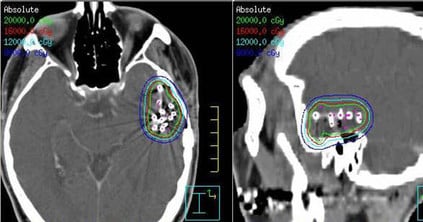
 Researchers at the Broad Center of Regeneration Medicine and Stem Cell Research on the Parnassus Campus of the University of California San Francisco have just published the results of two related studies involving differentiated brain cells transplanted into mice. In one case, the cells were human brain cells integrated successfully into a mouse brain; in the other, epileptic mice were cured with specialized mouse brain cells. In both studies the differentiated cells were a type of interneuron progenitor called medial ganglionic eminence (MGE) cells. Unlike other brain stem cells that can turn into any number of specialized cells, these differentiated MGE cells have a specific function, which is to inhibit signaling in overactive nerve circuits. These experiments hold promise for future treatment of neurological disorders like Parkinson’s disease, Alzheimer’s, epilepsy, and the chronic pain and spasticity caused by spinal cord injury.
Researchers at the Broad Center of Regeneration Medicine and Stem Cell Research on the Parnassus Campus of the University of California San Francisco have just published the results of two related studies involving differentiated brain cells transplanted into mice. In one case, the cells were human brain cells integrated successfully into a mouse brain; in the other, epileptic mice were cured with specialized mouse brain cells. In both studies the differentiated cells were a type of interneuron progenitor called medial ganglionic eminence (MGE) cells. Unlike other brain stem cells that can turn into any number of specialized cells, these differentiated MGE cells have a specific function, which is to inhibit signaling in overactive nerve circuits. These experiments hold promise for future treatment of neurological disorders like Parkinson’s disease, Alzheimer’s, epilepsy, and the chronic pain and spasticity caused by spinal cord injury.
Tags: 2014, CA, University of California San Francisco, 2013, University of California San Francisco Mission Bay, University of California San Francisco Parnassus, Parkinson's Disease Research, Southwest, California, University of California, brain research, San Francisco, SFVS, Biotechnology Vendor Showcase, UCSF, Parnassus, Mission Bay
Given the widespread use and abuse of alcohol for recreation, a drug that could interrupt its effects would have enormous value in treating alcoholism. Since addiction is based on stimulating pleasure centers, scientists have been looking for a way to block that interaction between alcohol and the brain. The challenge has been to find a key protein that carries out this transmission and identify its binding site. Now, biologists in the Harris Lab at the University of Texas Austin have made a major research breakthrough validating the importance of certain ligand-gated ion channels in that process and locating a cavity where the binding takes place. Remarkably, they were able to push their research forward thanks to an obscure alpine cyanobacteria recently sequenced in France.
Tags: 2014, 2013, University of Texas, Southwest, UTAust, alcoholism research, brain research, biology research, bio research, Austin, BioResearch Product Faire Event, TX
 The Fred Hutchinson Cancer Research Center and the University of Washington Medicine in Seattle are pleased to announce the arrival soon of Dr. Eric Holland, a world-class brain cancer research scientist and neurosurgeon, who will head up the Human Biology Division at Hutch as well as the Alvord Brain Tumor Center at UW. The eminent MD/PhD is being lured away from Manhattan's Memorial Sloan-Kettering Cancer Center, where he directs the MSKCC brain tumor center and has his lab within the Cancer Biology and Genetics Program, where his team studies the molecular mechanisms underlying the development of central nervous system tumors. In addition to being the recipient of many prestigious awards over years, Holland brings with him over $3M a year in NIH/NCI funding. It's unclear how many of his 13 lab members will follow him across the country to take on new challenges at Hutch and UW.
The Fred Hutchinson Cancer Research Center and the University of Washington Medicine in Seattle are pleased to announce the arrival soon of Dr. Eric Holland, a world-class brain cancer research scientist and neurosurgeon, who will head up the Human Biology Division at Hutch as well as the Alvord Brain Tumor Center at UW. The eminent MD/PhD is being lured away from Manhattan's Memorial Sloan-Kettering Cancer Center, where he directs the MSKCC brain tumor center and has his lab within the Cancer Biology and Genetics Program, where his team studies the molecular mechanisms underlying the development of central nervous system tumors. In addition to being the recipient of many prestigious awards over years, Holland brings with him over $3M a year in NIH/NCI funding. It's unclear how many of his 13 lab members will follow him across the country to take on new challenges at Hutch and UW.
Tags: 2014, 2013, Northeast, Fred Hutchinson Cancer Research Center, Washington, UW, University of Washington, WA, Northwest, cancer research, Memorial Sloan-Kettering Cancer Center, brain research, Neuroscience, BioResearch Product Faire Event, Funding, Front Line event, Seattle, Frontline Event, Hutch, Cancer Center
 Neurobiology research has a long and storied history at Columbia University and its Medical School in New York, dating back to the groundbreaking work of American neurologist Harry Grundfest 60 years ago. 30 years ago Columbia became one of the first universities to bring together diverse, cross-disciplinary researchers in neighboring labs to study behavior at the cellular, molecular, and systems level. By 2004, when Columbia celebrated its 250th anniversary, university president Lee Bollinger (right) announced the formation of a Mind Brain Behavior Initiative to more productively bring scientists into an even more integrated research effort across not only the two existing New York City campuses, but with an anchor (and crossroads) at the new CU Manhattanville campus then in the active planning stages.
Neurobiology research has a long and storied history at Columbia University and its Medical School in New York, dating back to the groundbreaking work of American neurologist Harry Grundfest 60 years ago. 30 years ago Columbia became one of the first universities to bring together diverse, cross-disciplinary researchers in neighboring labs to study behavior at the cellular, molecular, and systems level. By 2004, when Columbia celebrated its 250th anniversary, university president Lee Bollinger (right) announced the formation of a Mind Brain Behavior Initiative to more productively bring scientists into an even more integrated research effort across not only the two existing New York City campuses, but with an anchor (and crossroads) at the new CU Manhattanville campus then in the active planning stages.
Tags: 2014, 2013, Northeast, New York, Columbia University, brain research, Neuroscience, Columbia, BioResearch Product Faire Event, Funding, Neurology, NY, New York City, Northeast Region, charitable giving
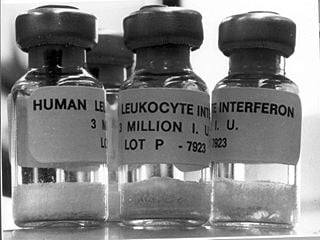
Researchers in the St. Giles Laboratory of Human Genetics of Infectious Diseases at Rockefeller University have recently published the results of a study that demonstrates how organs like the brain have their own defense systems which, when disrupted, can permit disease despite a healthy white blood cell count. The key is the production of interferon, which are proteins triggered by a receptor called TLR3 that send up the alarm to fight infection (by interfering with the pathogen's reproduction). When that TLR3 receptor is faulty on a neuron or other brain cell, no interferon is produced and the patient can suffer a disease of the brain even though that same pathogen is being combatted effectively in other parts of the body. We now know there seem to be localized systems of immune response within specific organs, and that interferon therapy may help patients with rare localized diseases.
Tags: Rockefeller University, biomedical research, Stem cell research, New York, 2012, Immune System, brain research, BioResearch Product Faire Event, NY, New York City